Introduction
Australasian plastic surgery has a history of involvement with international pro bono surgical programs to assist developing nations in the management of congenital and acquired conditions. Cleft lip and palate surgery has been the focus of many of these. Following the earlier lead by the United States, Interplast Australia was formed in 1983 and has had a proud record of running many surgical and educational programs in over 25 countries of the Asia-Pacific region.1 Less publicised but also significant have been the efforts of other groups and individuals who have performed similar work. One such group, now under the umbrella of Open Heart International2 has visited Nepal on an annual basis since 1994.
Nepal is a nation whose land mass is about twice the size of Tasmania and encompasses large parts of the Himalayan Mountain chain. Apart from the capital Kathmandu, as of mid-2017 the population of approximately 30 million3 is concentrated in small towns and villages, often in very remote areas in altitudes up to and over 3000 metres. Winters at altitude can be extremely cold, requiring heavy clothing, traditionally of yak’s wool, but more recently of more flammable synthetic fibre. A large part of the population lives in basic housing of brick or wood with thatched roofs and dirt floors. Cooking is usually done with kerosene or gas bottle stoves, often on the floor of the communal living area. Children run freely in these areas. Accidents related to cooking are common, with toppled over boiling water pots, hot oil and house fires being the cause of a very high rate of burn injury. Immediate medical treatment is rare and both mortality and long-term morbidity from burns is much higher than in developed countries. Many communities only have access to basic medical facilities by walking several days, even before they reach a road. Peripheral hospitals able to treat burns are few.
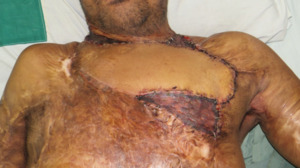
As a result, those patients who survive significant burn injuries frequently develop deforming burn-scar contractures of a severity rarely seen in developed nations (Figure 1). Many of these victims lose the capacity to work and become either totally dependent on family or end up on the streets as beggars. In a country where the power grid is switched off twice daily, surgical treatment in government facilities is unavailable to the vast majority of people.
Nepal also has a high rate of cleft lip and palate deformity. Surgical treatment of this condition has attracted many overseas missions to offer surgical repair to these patients. One of these surgical missions originated with the work of Dr Charles Sharpe from the Sydney Adventist Hospital. From 1994 on, Sharpe led an annual team of plastic surgeons, anaesthetists and nurses to offer cleft lip and palate repair in a clinic in the town of Banepa, situated approximately 25 km east of Kathmandu. The clinic was set up as a day surgery/short stay surgery centre inside a building housing a relief agency (Adventist Development and Relief Agency—ADRA). It had to be set up as a surgical centre ‘from scratch’ with equipment transported from Australia on each occasion. Over 600 patients were thus treated over the ten years to 2004.
As is often the case in developing nations, any medical program set up for whatever purpose is soon overrun with patients living with conditions unrelated to the original aim: in this case, cleft lip and palate. Some of the conditions often seen by Sharpe’s team were severe burn-scar contractures. Aware that a short stay surgery centre was not appropriate for these patients, Sharpe negotiated with the nearby Scheer Memorial Hospital (SMH) to set up a burn-scar contracture program, which the author was invited to run. In April 2004 simultaneous cleft lip and palate and burn-scar contracture programs were run by a combined team at the ADRA Nepal building and the nearby SMH.
Initially the the pilot burn-scar program was run solo, utilising the anaesthetic and nursing staff of SMH and with the help and advice of Nepali plastic surgeon, Dr Shankar Man Rai. Thirty-one patients were operated on in the course of ten days.
During much of the time of the cleft program, Nepal suffered from a long-standing guerilla campaign by Maoist insurgents. Their influence with the population frequently led to ‘ban’ days, amounting to a general strike. The government’s reaction was to call a military daylong curfew, with threats to shoot anyone seen on the streets. These frequent disruptions made the running of surgical programs not only difficult but also dangerous. In 1999 the ADRA building used by the cleft team was bombed, with a staff member suffering severe barotrauma to her ears. Another bomb shattered all the windows of a hotel block where the 2004 team stayed. The political situation further deteriorated when, on 1 February 2005, King Gyanendra imposed martial law for the second time since 2002, dissolved parliament and sealed off the Kathmandu valley. This was not to last, but the next few years were extremely unstable, with frequent riots that finally resulted in the king turning over power completely to an elected coalition and re-instating the House of Representatives in April 2006.
In 2005, at the invitation of SMH, a small team of Australian nurses had visited to assess whether a regular burn-scar surgical program could commence in 2006. The 2006 program was initially postponed due to civil strife, but commenced in a small way immediately after King Gyanendra relented and peace was restored in April 2006. As the political situation became much more stable, and despite some continuing difficulties, the team returned to Nepal in April each year thereafter.
The Australian cleft program ceased in 2004 but cleft surgery continued with a team from Japan, transferred to the SMH on a twice-yearly basis. Up until the time of writing, the burn-scar program has continued with the services at various times of three Australian plastic surgeons, one from New Zealand, a Nepali plastic surgeon, several Australian assistant surgeons, four Australian and one Japanese anaesthetist. Each time a dedicated team of nurses from all over Australia assists the staff of SMH in caring for our patients. For most of this period the program was coordinated by the former nurse unit manager of plastic surgery at the Sydney Adventist Hospital, John Sanburg.
A simultaneous program of nurse education by senior Australian nurse educators was usually undertaken to train the nursing staff of the SMH. All team members paid their own travel and accommodation costs.
Another common surgical complaint in Nepal is uterine prolapse. In 2010 an Australian gynaecological team co-located at SMH with the plastic surgery team, offering women surgical repair of this debilitating condition. They benefitted from the methodology and logistics developed by the burn team. From 2013 onwards, the teams arrived ‘back-to-back’ so as not to overwhelm the hospital with the case load.
The author retired from the plastic surgery team after 2014. This is a report on ten successive plastic surgical missions between 2004 and 2014. There have been further team visits in 2015 and 2016, but due to several difficulties, the future of further team visits is in doubt.
Patient assessment
Assessment of suitability for surgery gradually evolved over the ten years of the program. Initially we relied on field assessments undertaken through the year by a lay field worker from ADRA Nepal. Field workers itinerated across Nepal, offering humanitarian aid and some basic medical help, such as the distribution of clean birthing kits to expectant mothers. These visits to the villages usually resulted in the aid worker being swamped with people suffering from various ailments, including many burn-scar contractures. He would take details of those whom he thought might benefit from surgery, but he being medically unskilled, frequently patients would be selected for the program who would not benefit from surgery.
Because the field assessment process was somewhat unreliable, after a few years the field worker was encouraged to take digital photographs of each potential patient’s deformity as well as their name and contact details. Photos were then emailed to the principal surgeon (the author) back in Australia, who would then assess the likelihood of success from surgery. This greatly refined the selection process so that non-starters would not travel large distances, only to be rejected as unsuitable. It also allowed more efficient planning of theatre time and length of patient stay in advance of the team’s arrival.
It was not unusual to have more than 100 potential patients arrive at SMH for assessment and many had travelled long distances. Usually on the afternoon of the team’s arrival in Nepal, an assessment clinic was set up in hospital premises with a number of stations. These consisted of registration of potential patients, assessment by the surgeons, anaesthetic assessment of those deemed surgically correctable, followed by photography and referral for pathology. As the tuberculosis rate in Nepal is high, anyone with a cough or cachexia had a chest X-ray and most patients had a haemoglobin level taken, as parasite infestation and anaemia are also common. Most patients were then given a dose of pyrantel to treat intestinal parasites.
Patient statistics
A total of 378 patients had primary surgery in this period. Total anaesthetic events were approximately 500, as many children and some adults had dressing changes, suture removal and minor debridement procedures under anaesthesia during their stay. The most common age group accepted for surgery was the second decade of life. In all age groups, females predominated (see Discussion).
As is usual in Asia, patients and relatives pay for their out-of-hospital accommodation, which is arranged by hospital staff, and averages about AU$1.00 per day. All hospital costs were met by the visiting team and were remitted to the hospital in bulk. No patient was charged for his or her treatment.
Local staff training
Hospital nursing staff had regular in-service training by the visiting team nurse educators, concentrating on wound care. The team was joined through most of the decade by an experienced local Nepali plastic surgeon, Dr Basant Mathema. He would often bring a junior colleague as a training experience. Two-way exchange of knowledge and camaraderie was one of the more pleasant aspects of the whole experience.
Conditions treated
Although the focus of the program was the surgical relief of burn-scar contractures, a small number of patients were treated for syndactyly or polydactyly and rarely for other congenital deformities such as epispadias. Several patients were referred to other centres with conditions not treatable by our team.
As of 2014, the total number of patients treated was 378, with an (estimated) 100 or more further separate procedures under anaesthesia under-taken as Table 1 shows.
A complete breakdown of all procedures for all years is not available from records kept. However, Table 2 shows a breakdown of patient diagnosis and procedure type for the years 2007–2011.
A snapshot of the types of problems treated over a three-day period from the 2012 program is shown in Table 3.
Procedures utilised with results
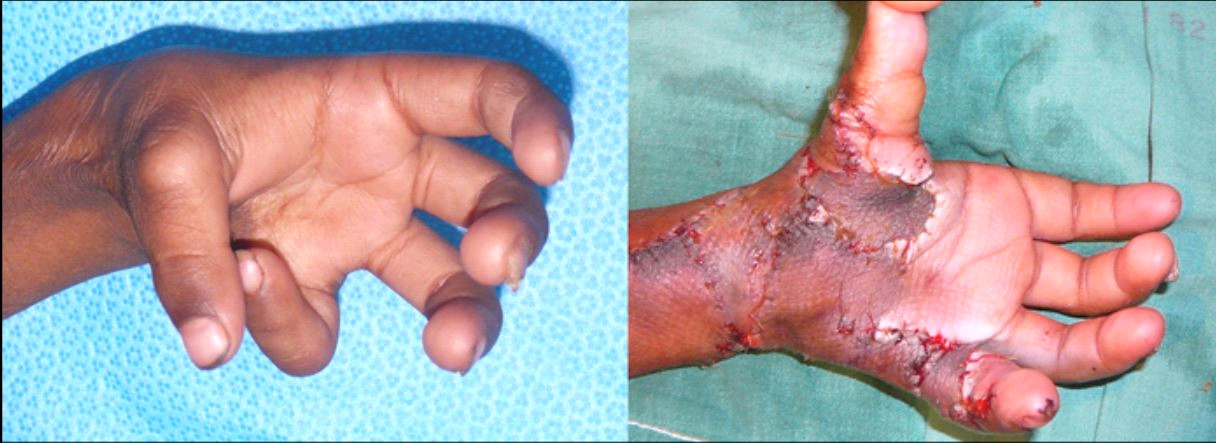
As can be seen in Table 2, the largest number of procedures involved full thickness skin grafts and the largest numbers of cases by far were contractures of fingers (Figures 2 and 3). Grafts were usually taken from the groin and closed primarily, except where burns had affected the groin areas. Most hand burns required relatively small grafts, but neck contractures and other sites such as shoulders often required very large grafts. Use of donor skin was often limited by scarring of donor sites, requiring opportunistic selection of non-standard donor sites. For example, in parous women a common donor site for large grafts, up to 40 cm by 15 cm wide, was the abdomen. Skin could be harvested by performing an abdominoplasty and de-fatting the excised pannus. With large grafts, quilting techniques were used extensively. Z-plasties were frequently employed, especially in long-standing contractures where skin stretching had occurred, or for minor contractures.
Flap choice sometimes required opportunistic selection of unusual donor areas, such as the island scapular flap or reverse radial forearm flap.
Neck and axillary contractures have bad reputations for recurrence after grafting (Figure 4). Neck contractures also face challenges for intubation and airway maintenance, as well as graft immobilisation. Consequently, in three patients over the whole program, latissimus dorsi flaps were used after the release of lower neck contractures and one for an axillary contracture (Figures 4, 5, 6). The first was a muscle-reduced flap, and the last two were true island perforator flaps. The first LD flap appears in Table 2. The other two were performed after 2011, so do not appear in Table 2.
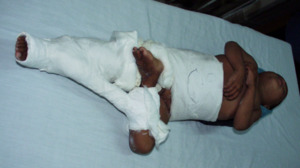
Microsurgery was not available due to equipment limitations, so some outdated procedures had to be resurrected for certain situations. Several cross-leg flaps and two cross-thigh flaps in infants or very young children were successfully performed (Figure 7). For severe palmar contractures, reverse radal forearm flaps were sometimes utilised (Figure 8), usually with anastomosis of a flap vein under loupe magnification to enhance venous drainage. Pedicled groin flaps were used for some hand contractures. Second-stage division of flaps at three weeks was undertaken by our local plastic surgical colleague.
Severe volar forearm contractures from childhood usually result in shortening of multiple flexor tendons. Relief of the skin contracture does not correct this problem. In two such patients (who presented as adults) the problem was solved by skeletal reduction of radius and ulna and internal fixation. Both patients achieved surprisingly good functional return, albeit with shortened forearms by up to four centimetres.
Complications
Due to the intense and concentrated nature of the surgical effort, high standards of record-keeping were difficult to sustain. Only major complications were recorded. The author attended every patient in the series either operatively or in the postoperative inpatient period on a daily basis, six days a week. There were no postoperative deaths. There were no admissions to intensive care facilities and no urgent transfers to other hospitals. Of ‘major’ complications, there was one loss of a digit due to circulatory inadequacy after extensive scar release. There was one complete loss of a major flap, a reverse radial forearm flap where venous anastomosis was not performed. No data is available for wound infections, but anecdotal experience revealed a remarkably low rate of serious wound infection. Single-dose prophylactic antibiotics (usually IV cephalosporin) were used extensively. Total graft loss was rare, but partial graft loss more common. This was partly due to the almost exclusive use of full thickness grafts. Minor flap loss, such as the tips of z-plasties, was relatively common, as expected in patients where the skin had been substantially damaged by scarring. Tip loss occurred in several two-stage flaps, but in only one did that cause failure of the intended procedure, due to separation of the flap from its inset.
Discussion
The unstable political situation of Nepal has meant that government regulation of industry and the policing of safety concerns have suffered. This is compounded by the weakness of the economy, as Nepal has few natural resources, a challenging climate and is earthquake-prone. The most important highway out of Kathmandu has been built using Chinese aid funds. Nepal has very few health and safety regulations. It is commonplace to see gas cylinders and fuel containers lying about houses. Petrol and diesel fuel handling can be haphazard and traffic control in the Kathmandu valley is nearly non-existent. Motor vehicle accidents where burn injuries occur, especially bikes, are common. Government regulation of dangerous practices causing burn injury seems a long way off. In recent years a 100-bed government burns unit has been established in Kathmandu; that also struggles with the large numbers of cases and limited resources available.4
Note has been made of the female predominance among our patients. One explanation of this could be the working role of women in Nepali society. Apart from the fact that they are invariably the cook of the household, and exposed to the risk of hot oil and boiling water, females are often the hardest workers. Gupta and colleagues5 found in a population-based study that the highest incidence was in the third decade and the commonest causes were scalds. Our peak numbers were in the second decade, but we confirm Gupta’s findings that scalding is the most common causative agent. Young girls are encouraged to learn cooking skills while brothers are outside kicking a ball or playing cricket. Women in this agrarian society dig fields, harvest crops and carry huge loads (hence the high incidence of uterine prolapse). Open fires to burn refuse are common. Spousal abuse is at least as common as in Australia, largely due to alcohol abuse, and can take severe forms, such as acid throwing. Criminal activity also contributes to burn injuries.6
A number of our patients returned for further surgery a year or more after their first procedure. Revision surgery, such as thinning of flaps, removal of implanted hardware (surgical plates), scar revision and further grafting of old or new areas were the usual reasons. The most notable example of these was a young woman who had sustained the most horrific facial scarring after falling face-first into a fire after an infantile seizure. When first seen in 2008, she was facing blindness from exposure of her corneas, unable to close her eyelids and suffering constant painful episodes of conjunctivitis and keratitis. She was an outcast with little hope of marriage or employment. Urgent release of her lower eyelids with large skin grafts relieved her circumstances. Over the subsequent four years this patient returned another three times for extensive release of facial scars and full thickness grafting with a pleasing outcome. At her last visit she had improved in appearance, was married and spent much of her time smiling. With regret, as patient consent cannot be obtained due to time and distance, photographs illustrating her progress cannot be used.
Conclusion
The ideal solution to the problem of burn-scar contracture is prevention. This requires a national effort of re-education, the application of domestic and industrial standards of equipment safety and handling practices, such as those that exist in developed nations, and the availability of modern treatment centres for acute burns. The bottom line is monetary cost, something most developing economies struggle with.
For the present, however, reconstruction of burn-scar contractures in developing nations often involves unique conditions that challenge the ingenuity and resourcefulness of those who accept the challenge. Lateral thinking is often needed. The well-known Australian characteristic of finding simple solutions to complex problems (‘tie it up with wire’) comes to the fore. This is true in the ward as well as the operating theatre. Our teams often faced the situation of twice-daily blackouts (usually, but not always with generator backup), flies invading the sterile areas of theatres and equipment that had long ago ‘seen its day’. A sense of humour and team camaraderie needs constant refreshment. A grateful clientele of patients and families, smiles where tears used to be, hugs, presents of food, light-hearted games of cricket with patients in the courtyard, the traditional ‘night out’ in Kathmandu … all of these contribute to success. And that success saw team members return year after year.
Our experience is a microcosmic reflection of the massive global challenge of health in developing nations. This problem results from uncontrolled population growth, poverty, lack of education, crop failure and starvation, war and civil unrest, overstressed natural resources, unequal distribution of wealth, corruption, inadequate numbers of trained health professionals and a myriad of other causes. International aid efforts by many agencies are but a band-aid solution, so long as these root causes persist. But when all you have is a band-aid, you use it.
Acknowledgements
The author wishes to acknowledge Dr Charles Sharpe OAM FRACS and John Sanburg RN who assisted in the preparation of this article.
Consent to publish
Verbal consent to photography was granted to the author at the time of treatment.
Disclosure
The author has no conflicts of interest to disclose.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Revised: October 30, 2017 AEST





.png)






.png)