Introduction
Dermal substitutes play an integral role in providing physiological wound cover for major burns. NovoSorb (PolyNovo Biomaterials Pty Ltd) biodegradable temporising matrix (BTM) is a synthetic dermal matrix comprised of a 2-mm-thick sheet of biodegradable polyurethane foam bonded to non-biodegradable polyurethane sealing membrane. Following delamination of BTM and autologous skin grafting, the polyurethane foam is broken down by hydrolysis over 12 months without production of toxic by-products.1
We describe the technique of staged BTM and split thickness skin graft (STSG) for extensive hypertrophic facial burn scars in a young, cosmetically conscious patient, with a paucity of donor sites for full thickness skin graft (FTSG) harvesting.
Case
A 29-year-old female was retrieved to the Adult Burns Unit at the Royal Adelaide Hospital with 73 per cent total body surface area (TBSA) burns (70% full thickness truncal and 3% mid-deep dermal facial) and severe inhalational injury. The aetiology was flame burn with accelerant. No other traumatic injuries were noted on initial assessment. Full thickness burns covered the anterior neck, chest, abdomen, circumferential upper limbs and proximal lower limbs. Her facial burns were deep dermal thickness and extended confluently from her neck to frontal scalp.
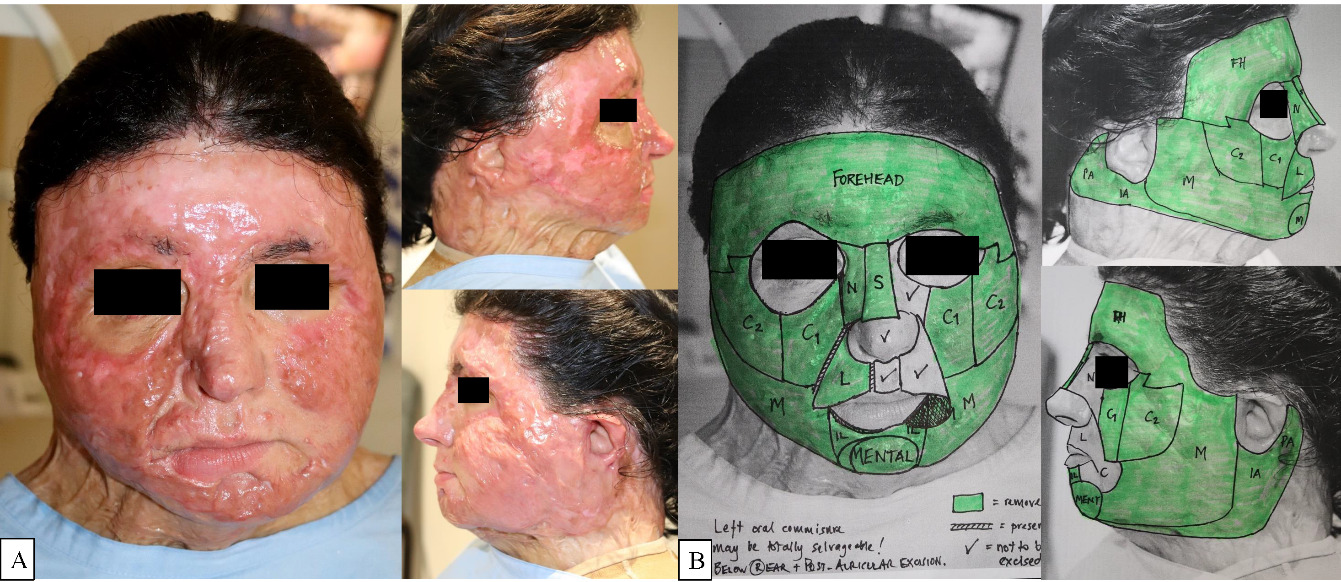
The patient presented to the emergency department alert and fully conscious, with clinical features of progressing inhalational injury. Following endotracheal intubation, escharotomies to bilateral upper limbs and chest were performed. Following subsequent multidisciplinary critical care management and fluid resuscitation, haemodynamic and thermal stability permitted major surgery. The patient underwent immediate total debridement of the 70 per cent TBSA full thickness burns. Dermal substitute application (BTM) occurred 48 hours after admission, in line with our departmental protocol for early burn wound excision in major (>50% TBSA) burns. The facial burns were managed conservatively with regular face care and paraffin ointment, as they were originally assessed as mid-deep dermal, in order to preserve as much viable dermis as possible. However, during the patient’s ICU stay she received high dose inotropes with subsequent progression of facial burn depth. Protracted facial burn wound healing over 8–10 weeks followed in the context of extensive burn injury and poor physiological state. Upper and lower eyelid burn scar contracture release with FTSG were the only early surgical facial burn interventions carried out to manage acute bilateral ectropion. Eventual facial burn wound healing was complicated by dense hypertrophic scarring that progressed over 12 months post injury and was associated with severe itch and discomfort (Figure 1). Itching was refractory despite trials of pharmacotherapy including cetirizine, amitriptyline and pregabalin. The inpatient treatment course was complicated by multiple infections (respiratory, urinary and line sepsis), iliac deep vein thrombosis secondary to femoral vein central venous catheter and a left frontal cerebrovascular event with dense right-sided hemiplegia. The patient was discharged to an inpatient stroke rehabilitation facility after a stay of 172 days on the acute burn unit, with the first 46 days spent in the ICU and 39 days ventilated due to inhalation injury and subsequent ventilator-associated pneumonia.
After 12 months of facial scar management and maturation post healing, the patient’s pruritis progressed leading to psychological distress and insomnia. Her facial scar hypertrophy failed to improve, measuring >1 cm in areas of greatest thickness as measured on high resolution ultrasonography. Burn wound excision was deemed necessary due to ongoing diffuse facial scar hypertrophy despite maximal multimodal therapy with scar massage, moisturising, silicone sheeting, soft and hard mask pressure garments, and ancillary procedures. The patient was counselled by the multidisciplinary burn team regarding the risks and complications of surgical facial burn wound excision with the goals of improving scar hypertrophy, pruritus and recurrent bilateral ectropion, despite early lower lid FTSGs.
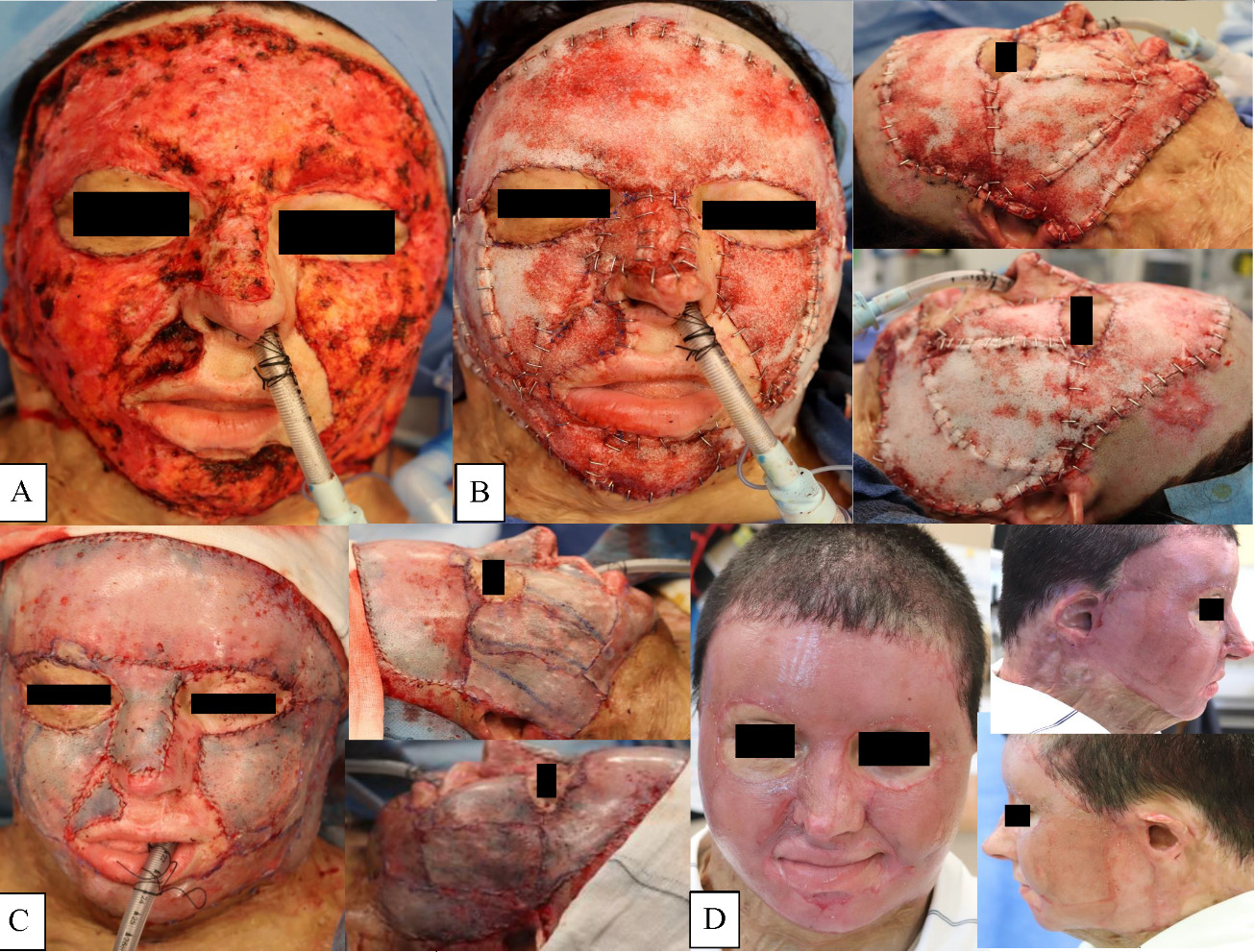
Facial burn scar reconstruction was planned in two stages. Hypertrophic facial burn scar excision and BTM implantation was carried out at the first stage. Delamination of BTM and application of autologous sheet STSG harvested from the scalp was carried out at the second stage, once BTM had integrated to the wound bed four weeks following its application (Figure 2).
Overall graft take was excellent (Figure 3) with no early perioperative complication. At 2.5 years post facial burn revision, the patient reported persistent, but greatly improved, mild itch affecting all burn scars, and mild recurrent right lower lid ectropion. Currently, she is receiving ongoing treatment with CO2 laser to the right cheek and neck for recurrent hypertrophic scar management, which appears subjectively less severe compared with her early burn scar prior to BTM reconstruction.
Discussion
Facial burn scars present a complex reconstructive and rehabilitative challenge for burns surgeons and therapists alike. Given the visible nature of the face, scarring in this location can negatively impact on function (including facial expression), cosmesis, quality of life and identity.2 Thus, the desired result is a scar of the highest quality possible.
Our department has developed significant expertise in the use of BTM throughout its development from initial animal studies to recent human clinical trials. Two-stage BTM reconstruction has proven robustness in scar contracture compared with other popular dermal matrices.3 It physiologically covers complex excised burn wounds, allowing for early rehabilitation and excellent scar cosmesis.
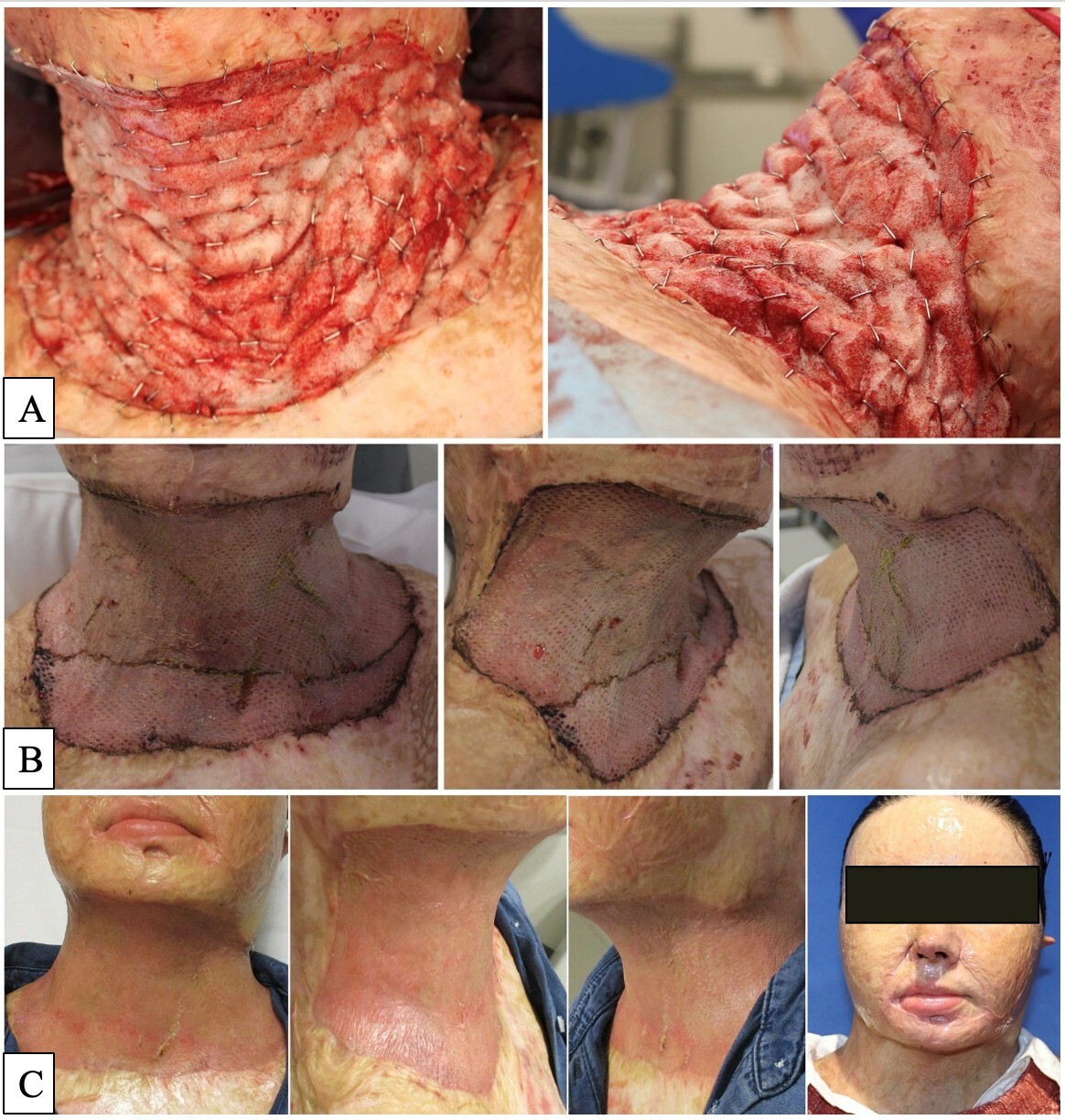
Ancillary procedures such as scar contracture release with local flaps or Z-plasty, corticosteroid injections and CO2 laser, brought about minor improvements for the patient’s facial scarring. However, the most dramatic improvement in appearance was noted following staged surgical revision of the face and neck with BTM and autograft. Prior to intrinsic facial scar excision and BTM application, we carried out extrinsic neck scar contracture release and sheet graft to eliminate any contribution of extrinsic neck tension to recurrent facial scar hypertrophy. Repeat release of neck scar contracture release and BTM/1:1 meshed autograft was required due to recurrent neck contracture. The second neck scar release, including platysmectomy, had a very beneficial effect on the patient’s facial aesthetics due to a pleasing release of caudal tension on the facial soft tissues and skeleton (Figure 3).
Several uses of dermal matrix for acute and secondary reconstruction of facial burns have been described by multiple authors.2,4,5 Gurbuz and colleagues6 comment ‘the use of dermal substitutes in the acute phase of burn treatment increases the amount of dermal component, and improves skin graft quality.’7–10 In-vitro studies of BTM demonstrate superior vascularisation when directly compared to other dermal substitutes.2 The completely synthetic composition of BTM appears to confer some resistance to matrix loss due to infection, permitting its success in large defects post resection of necrotising fasciitis.11 However, with respect to dermal matrices, detail on rebuilding and reconstructing facial subunits is limited. Therefore, this case report is highly important for use in future practice.
Facial aesthetic subunits are the primary structural areas of the face separated by natural folds and borders. These units comprise skin with similar histology, thickness, colour, texture and hair distribution. For optimal cosmetic outcomes, incisions and suture lines are best placed along cosmetic unit junctions without violation, allowing resulting scars to be less perceptible. The case reported in this pictorial review illustrates the successful use of BTM for hypertrophic facial burn scar reconstruction using a facial aesthetic subunit approach, with good cosmetic and functional improvements. Disappointingly, the application of BTM in cosmetic subunits did not confer a long-lasting result, as subunit junctions became obscured over time (Figure 3C). The loss of facial subunit definition may have occurred due to the diffuse nature of facial scarring in combination with the recurrence of scar hypertrophy, particularly at the right cheek, nasolabial fold and perioral regions where the initial burn was deepest and slowest to heal.
Conclusion
Dermal matrices such as BTM play an important role in secondary facial burn scar revision and may achieve excellent results when applied in line with basic principles of facial aesthetic subunits.
Acknowledgements
Tanya Klotz, senior occupational therapist, for information regarding scar rehabilitation and pruritis questionnaire.
Patient consent
Patients/guardians have given informed consent to the publication of images and/or data.
Conflict of interest
Elizabeth Concannon received an educational travel grant from PolyNovo to attend the American Burn Association Burn Surgeon Forum in December 2023. PolyNovo had no involvement in patient selection or preparation of this case report or its submission for publication. The other authors have no conflict of interest to disclose.
Funding declaration
The authors received no financial support for the research, authorship and/or publication of this article.
Revised: November 24, 2024 AEST