Introduction
NovoSorb (PolyNovo Biomaterials Pty Ltd) biodegradable temporising matrix (BTM) is a bilayer synthetic dermal substitute, consisting of a porous polyurethane foam bonded to a non-biodegradable sealing membrane.1,2 Widely studied, BTM has been shown to be effective in the management of complex, often ungraftable wounds, including those resulting from trauma, burns and infection.1,2 Its durability, biocompatibility and reliability have been well documented, and case studies have reported promising outcomes in the reconstruction of cutaneous defects following excision of cutaneous malignancies.1,3 Furthermore, BTM has been used successfully in patients receiving adjuvant radiotherapy, with consistently favourable wound healing outcomes.3,4
This report describes the novel use of BTM to reconstruct a complex nasal cavity defect. To our knowledge, this is the first published case describing the use of BTM in the reconstruction of the nasal cavity following total rhinectomy for head and neck cancer. The patient, unsuitable for free flap reconstruction due to comorbidities and social factors, underwent successful resection and BTM reconstruction, followed by adjuvant radiotherapy. This case highlights the potential role of synthetic dermal substitutes in reconstructing complex head and neck defects and underscores the resilience and adaptability of BTM in the context of adjuvant radiotherapy.
Case
A 50-year-old male was referred to Sunshine Coast University Hospital in November 2023 with a diagnosis of T4aN0M0 nasoseptal squamous cell carcinoma (SCC). His past medical history included chronic obstructive pulmonary disease secondary to a significant smoking history, hypertension, type 2 diabetes mellitus and schizophrenia. The patient was initially scheduled for resection with reconstruction using free tissue transfer; however, on the day of the procedure he declined to proceed due to personal concerns and uncertainty about the surgery. The patient presented one month later seeking further management of the nasoseptal SCC. Given his complex medical history, poor functional reserve and inconsistent engagement with care, he was deemed unsuitable for free tissue transfer and the use of BTM was considered a safer and more feasible alternative.
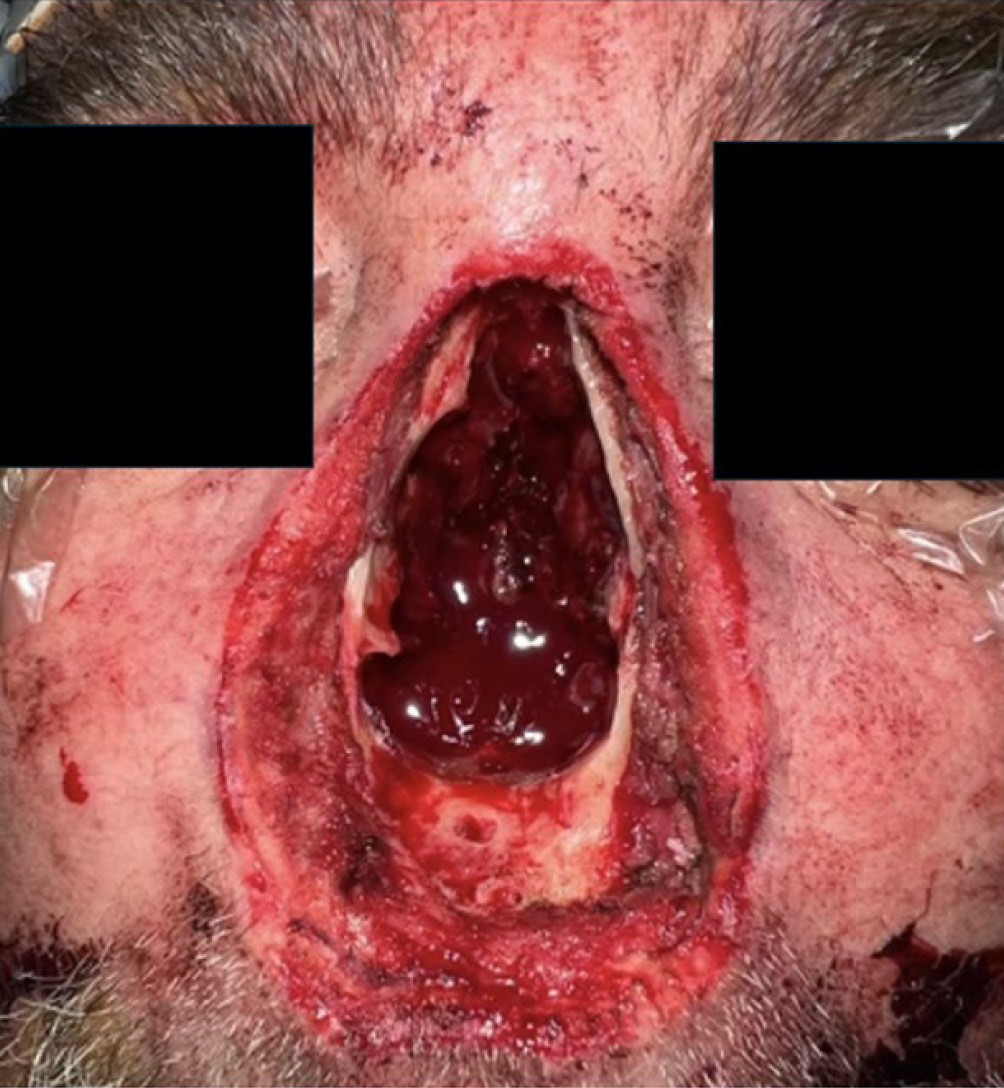
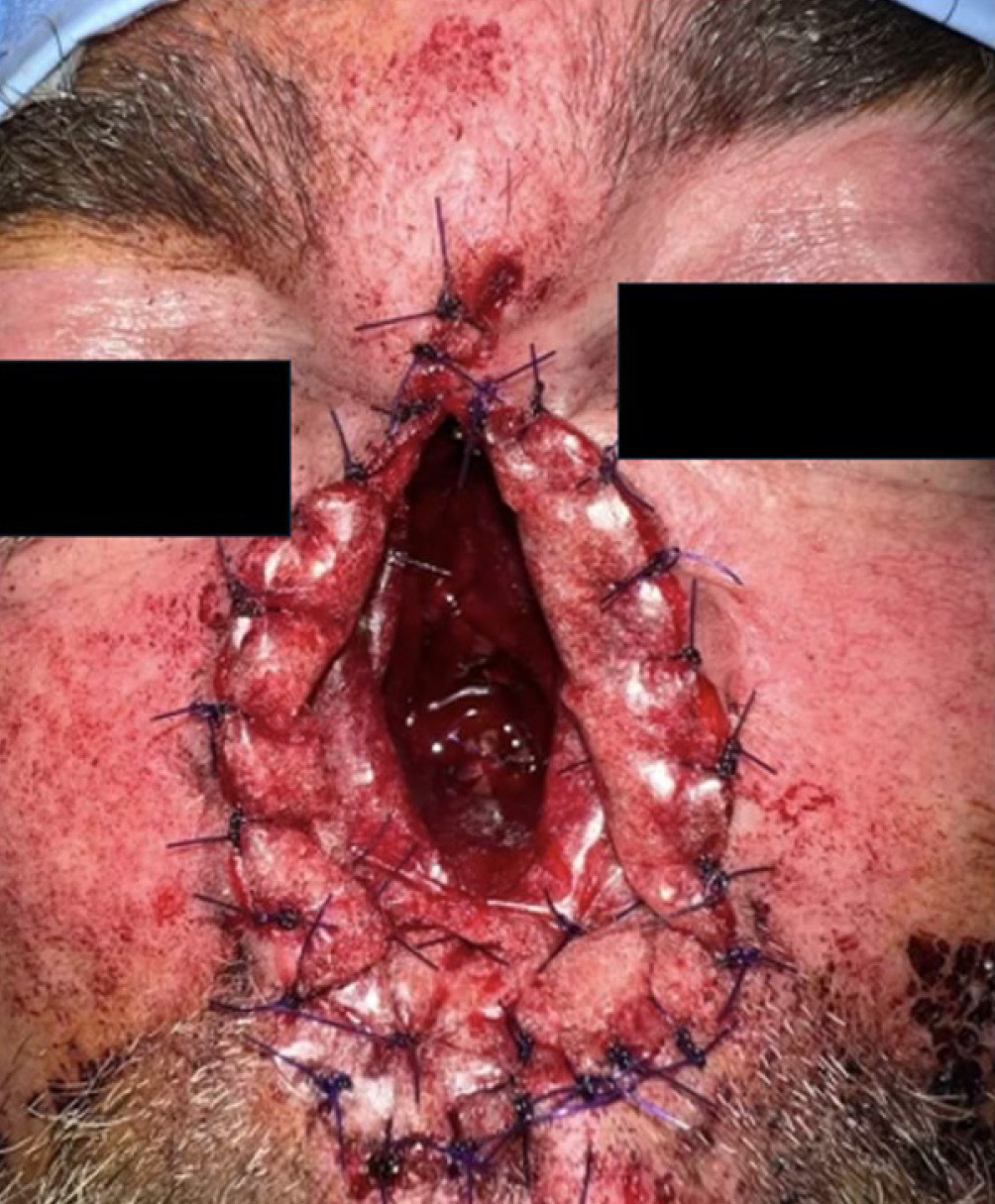
The patient subsequently underwent resection of the nasoseptal SCC, which involved a total rhinectomy, including resection of the nasal septum. The middle and inferior turbinates were split, and the mucosa and periosteum were stripped from the side walls and floor of the nasal cavity (Figure 1). The resulting defect was reconstructed with BTM, which was inset posteriorly to the remaining mucosa and anteriorly to the cutaneous margin. A bone drill was used to quilt the BTM to the hard palate and maxillae (Figure 2).
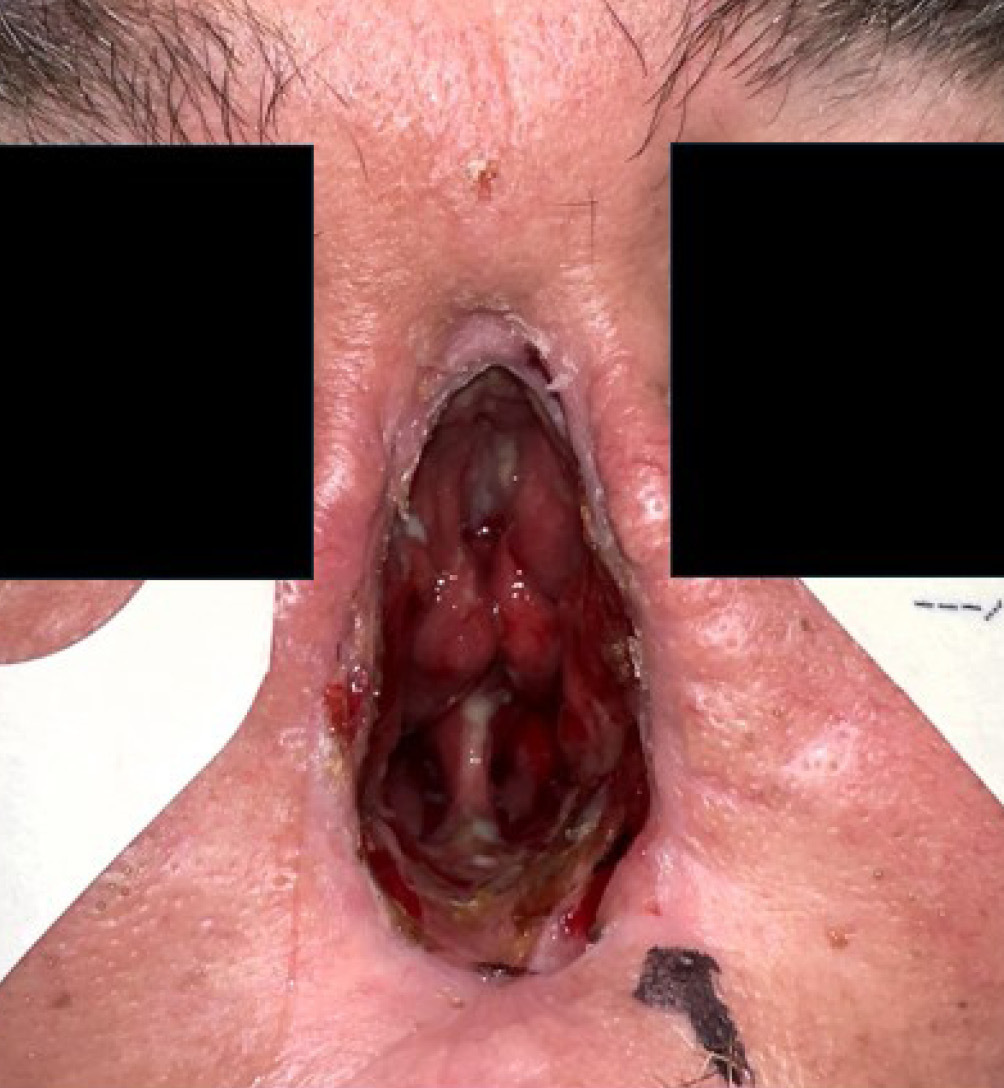
The patient commenced radiotherapy while the BTM laminate remained in place, receiving 60 Gy in 30 fractions. Sutures remained for four weeks, and regular flushing of the BTM was performed weekly to maintain wound cleanliness and minimise the risk of infection. Dressing alternatives that were explored, including packing the cavity to apply compression, were poorly tolerated. Radiotherapy was completed in April 2024 without complications and the patient proceeded to delamination two months later. Upon delamination, complete integration of the BTM was observed, along with full mucosalisation of the nasal cavity and no evidence of wound dehiscence or infection (Figure 3). Follow-up in July 2025 showed stable appearance of the nasal cavity following radiotherapy.
Discussion
The use of BTM in the reconstruction of complex wounds has been extensively studied, demonstrating that it is both reliable and versatile. Multiple case series have shown that BTM can successfully integrate over exposed bone and tendon—tissues traditionally considered ungraftable and requiring flap reconstruction.1,3,5 These reports have primarily involved the reconstruction of cutaneous defects in the context of burns, trauma and oncological resection.1–3,5 This case details a unique application of BTM, with its use in reconstructing a complex nasal cavity defect following resection of a nasoseptal SCC. In addition, this case adds to the current evidence that BTM has the potential to be used as a single stage reconstructive option, a technique that has been documented in cutaneous reconstruction.6,7 To our knowledge, this is the first reported case using BTM to reconstruct a mucosal cavity, in this instance a nasal cavity, further supporting the notion that BTM is a valuable and versatile option in the plastic surgeon’s armamentarium, particularly in anatomically complex or surgically challenging regions.
The management of advanced head and neck SCCs frequently involves adjuvant radiotherapy, which necessitates robust and durable soft tissue reconstruction. The use of BTM in the context of adjuvant radiotherapy has been explored. Buick and colleagues published a case in which a cutaneous forehead defect was reconstructed with BTM, followed by delamination and grafting prior to radiotherapy, with no reported wound breakdown during treatment.4 In contrast, Devine and colleagues reported a case series investigating BTM in reconstruction following the resection of cutaneous malignancies and found that up to 50 per cent of patients who underwent adjuvant radiotherapy required return to theatre due to failure of BTM integration.3 In the present case, the patient proceeded to radiotherapy prior to delamination. Although this required an extended period of nursing-supported dressings, it resulted in complete integration of the BTM and mucosalisation of the nasal cavity at the time of delamination. This outcome suggests that proceeding to adjuvant radiotherapy before delamination may be beneficial, potentially reducing delays to radiation and improving long-term wound outcomes. Further prospective studies are warranted to assess the safety and efficacy of this timing strategy, along with assessing if irradiated BTM may deteriorate over time.
Reconstruction of complex nasal cavity defects commonly involves free tissue transfer, such as a radial artery free flap, a technically demanding approach associated with prolonged operative time and extended inpatient stays for postoperative monitoring.8 Patients who are unsuitable for free flap reconstruction—whether due to comorbidities or complex social factors, as illustrated in this case—are often unable to access oncological resection, thereby limiting their treatment options. This case demonstrates that BTM may offer a viable alternative for nasal cavity reconstruction. It presents a technically simpler procedure with shorter operative time and no need for postoperative flap monitoring. The main drawback is the requirement for long-term, nursing-assisted wound care until delamination, which in this case was required over a period of four months. Local flap reconstruction of the nasal cavity, such as bilateral cheek flaps or bilateral nasolabial flaps, also represents a feasible option in comorbid patients and may facilitate more rapid wound healing, while reducing the need for prolonged nursing support, compared to BTM. However, the utility of local flaps may be limited in cases involving extensive posterior defects or in patients with compromised local tissue due to prior surgery or radiotherapy.
Conclusion
This case demonstrates the utility of BTM in the reconstruction of complex wounds, with no previous research exploring its use in nasal cavity reconstruction. It not only highlights the novel application of BTM but also underscores its robust nature, with complete integration and mucosalisation of the nasal cavity observed following adjuvant radiotherapy. Although free flap reconstruction is considered the gold standard for complex head and neck defects, BTM may serve as a viable alternative for patients who are unsuitable for free or local flap procedures, thereby enabling access to oncological resection and adjuvant radiotherapy.
Patient consent
Patients/guardians have given informed consent to the publication of images and/or data.
Conflict of interest
The authors have no conflicts of interest to disclose.
Funding declaration
The authors received no financial support for the research, authorship, and/or publication of this article.
Revised: June 29, 2025 AEST