Introduction
Cryolipolysis is a non-invasive technique for permanent, localised fat reduction and was first described in 2007.1 It is marketed as a safer alternative for removal of excess adipose tissue and body contouring, avoiding traditional invasive risks associated with liposuction.1 Based on principles of cold-induced panniculitis, whereby lipid-rich tissues are more susceptible to cold injury compared to the surrounding water-rich tissue, cryolipolysis relies on cold-induced apoptosis of fat cells translating to a measurable fat reduction.2
Current literature emphasises its overall safety and patient tolerability, with the majority of complications reported limited to erythema, swelling and minor discomfort to treated regions.3–5 There are, however, isolated reports of frostbite-induced cutaneous ulceration from direct thermal injury.6–9 These incidents were largely attributed to inexperienced service providers and faulty equipment, and are therefore relatively rare.
We report a novel case of a 26-year-old female who sustained an infected, full-thickness abdominal burn with underlying fat necrosis as a complication of her cryolipolysis treatment. This case should serve as a caution to patients and service providers of this potential risk and the possible complications that may ensue and, importantly, emphasise when to escalate care.
Case
A 26-year-old female underwent cryolipolysis to her abdomen at a private body contouring clinic utilising the Cooltech (Cocoon Medical, Carrer del Gall, 22, Esplugues de Llobregat, 08950 Barcelona, Spain) cryolipolysis device. It was set to a standardised temperature of −8 °C for 70 minutes. A cool gel pad anti-freezing membrane, as recommended by the manufacturer, was applied as an interface to prevent direct contact with the skin.
Two days following treatment the patient developed severe erythema, oedema and blistering within the treated area (Figure 1). She presented to her local emergency department and was discharged without referral to a specialist service, being reassured that the skin changes were self-limiting bruising. She received daily reviews at the original clinic, undergoing infra-red light-emitting diode laser treatment in conjunction with regular dressing changes. During this 12-day period, the abdominal skin became necrotic. At this stage, the patient was advised to self-present to the Victorian Adult Burns Service (VABS).
On admission to VABS, the patient was assessed as having a 2 per cent total-body surface area full-thickness abdominal burn with peri-wound cellulitis (Figure 2). She was commenced on empirical intravenous piperacillin/tazobactam and scheduled for operative intervention. During the first procedure, sharp debridement excised the full-thickness burn wound and associated fat necrosis underlying the abdominal eschar. In anticipation of repeated debridements and in the setting of concomitant infection, the wound was temporised with a negative pressure dressing. Tissue samples cultured multiple organisms including Stenotrophomas Maltophilia, Enterobacter Cloacae complex and Klebsiella Pneumoniae—her intravenous antibiotics were escalated to meropenem and cefepime. She underwent two further surgical debridement procedures. The wound was closed directly during her third operation once infection had resolved.
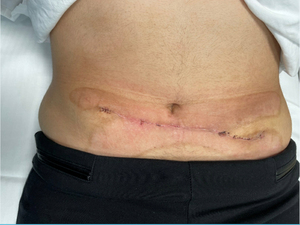
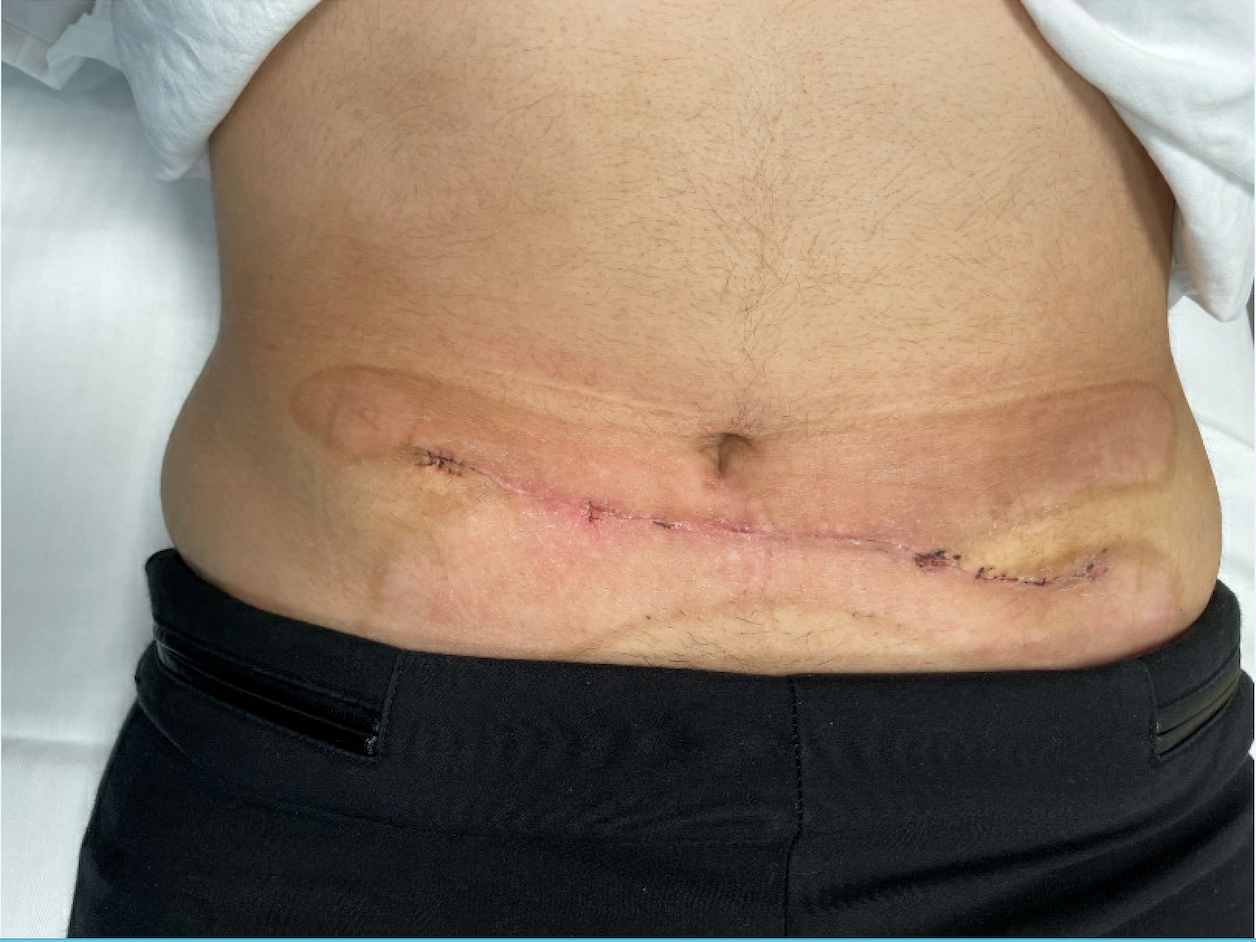
She was reviewed two weeks post wound closure in the outpatient clinic whereupon the wound was assessed as being well healed and demonstrating acceptable abdominal contour (Figure 3).
Discussion
Cryolipolysis and other non-invasive fat sculpting techniques are becoming more prevalent, driven by consumer demand for effective alternatives to traditionally invasive options. Cryolipolysis works on principles of cold panniculitis, where temperature facilitates selective apoptosis of adipocytes on isolated areas.2 Given the susceptibility of fat cells to respond to thermal changes preferentially to the overlying skin, it has been used for targeted fat reduction and body sculpting. An applicator with specialised freezing pads is set to a specific cooling temperature to target areas of the body. An antifreeze membrane is applied as an interface between the skin and the apparatus to prevent frostbite and thermal-related injuries.
Cyrolipolysis is marketed as a safe and effective procedure; the most commonly reported complications include bruising, swelling, erythema, pain and altered sensation. These complications are often minor, transient and self-limiting. In their review, Derrick and colleagues focused on the aforementioned short-term self-limiting complications noting an incidence rate of less than 1 per cent for all complications including localised decreased sensation and vasovagal reactions.10 A systematic review examining over 3000 patients similarly reported transient erythema, bruising and oedema as the most common adverse effects.7 These large studies have not identified any major safety signals, thus its overall safety is emphasised throughout the literature, which reverberates through mainstream marketing and media.
By its nature, cryolipolysis and other freezing treatments have an inherent risk of frostbite as freezing induces vasoconstriction, tissue hypoxia and thrombosis, which could lead to skin injury. Frostbite secondary to cryolipolysis has been reported in the literature with most authors owing this complication to user inexperience and technical equipment failures.6,8,9,11,12 The first such report described a 4 per cent full-thickness burn. However, this injury was sustained by a patient in a ‘do-it-yourself’ cryolipolysis attempt using dry ice at home.12 Subsequent reports have highlighted inappropriate use of the antifreeze membrane,11,12 with patients sustaining burn injuries requiring excision with closure and debridement and split skin graft respectively.9
Two further cases of frostbite injuries have been reported with the use of unregulated devices. The first case was a delayed presentation of a flank frostbite injury; the case was managed conservatively.6 The second case, also a flank frostbite injury, required a protracted surgical admission requiring multiple surgical debridement procedures.11 Hyperbaric therapy was used to improve tissue oxygenation, which reduced the size of the necrotic zone prior to surgical intervention.11 Reassuringly, despite the increasingly large number of cryolipolysis procedures performed worldwide, there have been few reports of frostbite-related injuries. These rare complications can be mitigated by maintaining equipment to required standards and ensuring it is used by experienced clinicians.
Our case is differentiated as the initial insult appeared to originate in the deeper layers, with the overlying skin initially spared and unlikely to be a cause of direct thermal injury. A possible hypothesis for the extent of this injury could relate to a direct perforator vessel injury, causing disruption to the entire volume of tissue it supplies. While the mechanism of injury remains inexplicit, there are several augmenting factors that should be highlighted which contributed to the morbidity experienced by our patient.
Firstly, the delayed presentation precluded the use of non-invasive treatment options, including topical glyceryl trinitrate ointment and hyperbaric oxygen therapy. Both therapies have been described to reduce the size of insult from cryolipolysis prior to surgical intervention. Secondly, the infra-red therapy was likely futile in this case—given the depth of initial injury—and may have compounded the injury. While surgical debridement was inevitable in this case, the delayed presentation and eventual infection contributed to the need for repetitive debridement surgeries and antimicrobial therapies.
As seen in our case, the notion of delayed medical assessment after initial injury is a recurrent factor observed throughout these cases, possibly related to a lack of awareness and appreciation of the severity of complications. Should complications arise, we advocate that service providers ensure a prompt assessment is made by a plastics, burns and reconstructive surgery service to provide optimal care.
Conclusion
While drawing conclusions on overall safety should be met with caution through an isolated incident, it demands heightened vigilance in all service providers and patients. This case illustrates a rare yet highly morbid complication of cryolipolysis, further augmented by suboptimal and delayed management in the post-injury period. In accordance with the increasing prevalence of these non-invasive contouring options, the spectrum of complications will increase. This is particularly relevant in a cohort where patients preferentially elect for cryolipolysis given its minimally invasive allure. In the setting of complications, early referral to a plastic, burns and reconstructive surgery service is recommended.
Patient consent
Patients/guardians have given informed consent to the publication of images and/or data.
Conflict of interest
The authors have no conflicts of interest to disclose.
Funding declaration
The authors received no financial support for the research, authorship and/or publication of this article.