Introduction
The kite flap, a pedicled fasciocutaneous flap based on the first dorsal metacarpal artery (FDMA), has been used to reconstruct a variety of hand defects including the dorsal thumb.1 Similarly, the extensor indicis proprius (EIP) tendon transfer is commonly used for extensor pollicis longus (EPL) tendon reconstruction.2 Tendon interposition arthroplasty is an evolving technique with potential application for the small joints of the hand, a field in which current existing surgical techniques suffer from various limitations.3 We describe a novel combination of these techniques, used to reconstruct a traumatic composite defect to the dorsal thumb with loss of the radial condylar head, segmental loss of the extensor pollicis longus tendon and the overlying soft tissue.
Case
A 76-year-old man presented after an angle grinder injury to his left thumb. He is right-handed and a non-smoker, with no previous medical history or reported history of arthritis.
In the operating theatre, examination revealed a 2 × 2 cm soft tissue and skin defect over the dorsal interphalangeal joint of the left thumb. Bone and joint were exposed, with a 2 cm segmental loss of the EPL tendon at its insertion. The dorsal surfaces of the proximal and distal phalanges were shaved off, involving 60 per cent of the radial condylar head of the proximal phalange. The collateral ligaments and nailbed sterile matrix were intact (Figure 1).
A handheld Doppler was used to mark out the course of the ulnar branch of the FDMA. A lazy S dorsal incision along the radial border of the second metacarpal was used for exposure. The EIP tendon was identified, before extending the incision distally towards the proximal interphalangeal joint (PIPJ) of the index finger. The flap was then raised, preserving the pedicle as well as the superficial venous vasculature where possible.
A longitudinal strip of extensor tendon proximal to the PIPJt was harvested in continuity with the EIP tendon and included in the flap. The flap, along with vascularised tendon, was then tunnelled subcutaneously as a single unit to reach the defect. A bone anchor was used to secure the transferred tendon with appropriate tensioning. The excess tendon length of approximately 2 cm was then buried in the condylar head space as a tendon interposition arthroplasty. The flap was inset with dissolvable sutures, and a full thickness skin graft was harvested from the volar forearm to repair the index finger donor defect (Figure 2).
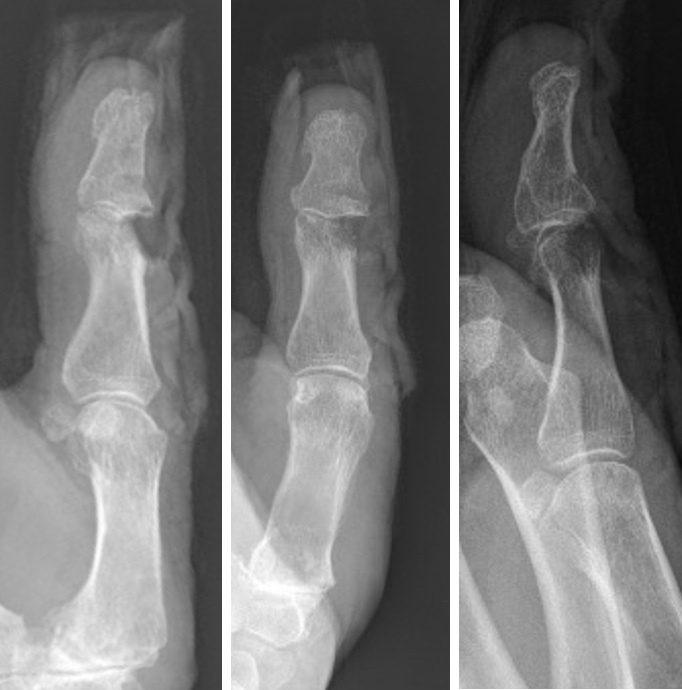
The index finger was splinted for a total of two weeks before commencing an active range of motion, and the thumb underwent standard EPL protocol with limited early active extension exercises and six weeks of extension splinting. Postoperatively there were no complications, with preserved extensor function of the index finger and no extensor lag. At four months, the patient had painless motion of the interphalangeal joint of the thumb, with full active extension to neutral position and 30° active flexion (Figure 3).
Discussion
In the highlighted case, our patient suffered a traumatic thumb defect requiring multiple elements of reconstruction. This particular injury allowed the neat combination of three well-established but usually separate techniques to reconstruct this composite defect with a relatively small incision and donor site.
The inclusion of a segment of vascularised extensor tendon with the kite flap for tendon reconstruction in the digits has been briefly described in the literature. In his reverse dorsal metacarpal artery flap series in 1990, Quaba described including a segment of extensor tendon in one case to reconstruct a missing distal segment.4 For thumb reconstruction, Sherif,5 and Karacalar and colleagues6 each described one reconstruction in which they successfully transferred the EIP tendon along with either the first or second dorsal metacarpal artery flap respectively.
The EIP tendon transfer is the most commonly used option to reconstruct the EPL tendon when direct repair is not possible. Extensor pollicis longus injuries usually occur at the level of the wrist or the musculotendinous junction, where a transferred EIP tendon can easily be pivoted to reach the intact distal stump for repair. Even in distal injuries, as in our case, EIP tendon transfer is still easily achievable but may require taking a longitudinal segment of the extensor tendon over the proximal phalanx to achieve the required length. This appears to have low donor morbidity, although the index finger may require a period of immobilisation, similar to the conservative management of a partial extensor tendon injury with a short period of splinting and early active motion.
The field of arthroplasty in the small joints of the hands for degenerative arthritis continues to be an evolving one. Current available surgical options, such as silicone or pyrocarbon implants, autologous toe joint transfer as well as soft tissue options such as volar plate arthroplasty, all suffer from a number of limitations. These include inadequate restoration of a painless range of motion, implant failure and significant rates of complication and revisional surgery.3
Tendon interposition arthroplasty as a technique has been commonly used in the hand and in particular, for the first carpometacarpal joint, a common example being the flexor carpi radialis tendon interposition combined with trapeziectomy and ligament reconstruction. Aslam reported using extensor retinaculum or palmaris longus interposition arthroplasty for the distal interphalangeal joint in a case series of five fingers, including one thumb, with good outcomes.7 In our case, we were able to use the additional length of our transferred tendon distally for interposition, bypassing the need to harvest tendon specifically for interposition. This is a simple but potentially valuable technique when restoring EPL function to an arthritic interphalangeal or metacarpophalangeal joint, as adding the tendon interposition component of the procedure is straightforward and requires minimal extra dissection. The tendon interposition could be performed even if a flap is not required for soft tissue coverage, but would require extending the incision distally onto the proximal phalanx of the index finger to achieve the required extra length of tendon for interposition.
Conclusion
Where indicated, the combination of EIP tendon transfer, kite flap and tendon interposition arthroplasty can be an elegant solution to reconstruct a traumatic thumb defect with minimal donor morbidity and excellent postoperative outcome.
Patient consent
Patients/guardians have given informed consent to the publication of images and/or data.
Conflict of interest
The authors have no conflicts of interest to disclose.
Funding declaration
The authors received no financial support for the research, authorship, and/or publication of this article.
Revised: December 16, 2021